As Finlay is currently undergoing medication for Cushings, we’re going to keep this “health issue” prominently placed. It is a disease which is becoming more and more common, but equally very easily over-looked by dog owners. Hopefully reading, and re-reading this article will help you understand what to look out for. If you currently have any doubts about the health of your dog, please don’t hesitate to make an appointment with your Vet. Articles like these throughout the web are only provided as “information” – the only place you can get the right help is by talking with your Vet. (article originally posted in November 2011)
 Cushing’s Disease in Scottish Terriers
Cushing’s Disease in Scottish Terriers
Cushing’s Disease in Scottish Terriers (and other breeds) is a common endocrinological disorder in dogs. In humans though, CD is rare. The clinical presentation of CD is however, is highly similar between both dogs and humans with characteristic signs such as abdominal obesity, weight gain, fatigue, muscle atrophy, and skin changes.
Harvey Cushing M.D. (8 April 1869 – 7 October 1939) was the first to discover the problems caused by the malfunction of the pituitary gland and in his report of 1912 termed it “polyglandular syndrome” later to become more famously known as: “Cushing’s Syndrome.”
Cushing’s Disease in Scottish Terriers and other dogs, is probably very easily overlooked by many Scottie dog owners as it is usually only associated with the elder Scottie and we therefore tend to think that it is the onset of old age.
You may already be familiar with Cushings Syndrome, but the details below will give you some vital information. Reprinted with kind permission from PetEduction.com
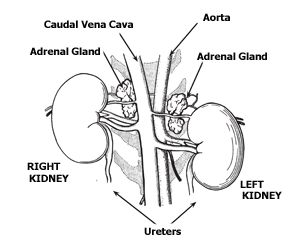 Cushing’s disease (hyperadrenocorticism) in dogs is a condition that results from the chronic overproduction of too much glucocorticoid in the body. In the normal dog, the pituitary gland produces a hormone called ACTH, which stimulates the adrenal gland to produce the glucocorticoid hormones necessary for the function of many systems in the body. If something goes wrong in the pituitary gland or adrenal gland and too much glucocorticoid is produced, then Cushing’s disease develops. This is a very complicated disease with a wide range of symptoms and causes. This article will try to give a concise description of the disease, its symptoms, how it is diagnosed, and its treatment.
Cushing’s disease (hyperadrenocorticism) in dogs is a condition that results from the chronic overproduction of too much glucocorticoid in the body. In the normal dog, the pituitary gland produces a hormone called ACTH, which stimulates the adrenal gland to produce the glucocorticoid hormones necessary for the function of many systems in the body. If something goes wrong in the pituitary gland or adrenal gland and too much glucocorticoid is produced, then Cushing’s disease develops. This is a very complicated disease with a wide range of symptoms and causes. This article will try to give a concise description of the disease, its symptoms, how it is diagnosed, and its treatment.
Who gets Cushing’s disease?
Cushing’s disease is considered a disease of middle age and older dogs and cats. It is much more common in dogs. This disease is similar in cats except that in cats up to 80% also have concurrent diabetes mellitus. This article will refer to the problem as it occurs in dogs. The usual age of contracting the disease is around six or seven years with a range of two to sixteen years. There is equal distribution between males and females and there does not appear to be an increase of the disease in any one breed.
What are the symptoms of Cushing’s disease in dogs?
| For dogs ultimately diagnosed with Cushing’s disease, hair loss was one of the most common reasons the owners first brought their dog in for evaluation. |
As a result of the chronically elevated glucocorticoids (steroids), the affected dogs develop a classic combination of dramatic clinical signs and lesions. The disease progresses slowly. A study showed that most dogs had at least one symptom of the disease from one to six years before the disease was diagnosed. Because the symptoms occur so gradually, the owner often attributes the changes to “old age.” Some dogs will have only one symptom, while others may have many.
Increased Water Consumption and Urination: The most common symptom is increased consumption of water and the resultant increased urination (polyuria/polydipsia). The dogs drink between two and ten times the normal amount of water and the resultant increase in urination follows. This symptom is present in over 85% of all animals with Cushing’s disease. Previously housebroken animals may begin to have accidents because their bladders fill quickly with the overproduction of urine.
Increase in Appetite: Increase in appetite (polyphagia) is another common clinical symptom that shows up in around 80% of the affected animals. Dogs may begin stealing food, getting into the garbage, begging continuously, and become very protective of their food. Despite having other symptoms, the owner may feel that the dog is okay because of his good appetite.
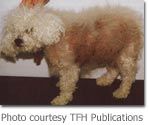 Abdominal Enlargement: Abdominal enlargement is a common symptom in up to 80% of the affected dogs. The potbellied appearance is a result of the shifting of fat to the abdominal area and a weakening and wasting of muscle mass in the abdomen.
Abdominal Enlargement: Abdominal enlargement is a common symptom in up to 80% of the affected dogs. The potbellied appearance is a result of the shifting of fat to the abdominal area and a weakening and wasting of muscle mass in the abdomen.
Hair Loss and Thin Skin: Hair loss and thinning of the skin are also common symptoms in dogs with Cushing’s disease. It is estimated that between 50% and 90% of the affected animals develop these symptoms. Hair loss (alopecia) is one of the most common reasons that owners bring their dog in for evaluation. The hair loss usually starts over the areas of wear such as the elbows and progresses to the flanks and abdomen until eventually only the head and extremities have hair. The skin may also become thin and be easily damaged and slow to heal.
Increased panting, recurrent urinary tract infections, or losses in reproductive ability are other symptoms often noted with this disease.
Cushing’s Disease has two forms
There are two different distinct forms of the disease. There is pituitary dependent hyperadrenocorticism (PDH) and there is an adrenal-based disease.
Pituitary dependent hyperadrenocorticism: PDH involves the oversecretion of ACTH by the pituitary gland. ACTH is a hormone that stimulates the adrenal gland to produce glucocorticoids. The pituitary gland is most likely overproducing ACTH because of a pituitary tumor. The PDH form of the disease is responsible for around 80% of the cases of canine Cushing’s disease.
Adrenal-based hyperadrenocorticism: The adrenal-based form of the disease is usually a result of an adrenal tumor that causes an oversecretion of glucocorticoids. Adrenal tumors are responsible for around 20% of the cases of Cushing’s disease. There is also a form of the disease called “iatrogenic” Cushing’s disease that occurs as a result of giving the animal high doses of steroids. In this form of the disease, symptoms of Cushing’s disease will go away once the steroids are discontinued.
Diagnosis
| It is recommended that any dog suspected of having Cushing’s disease should have a complete blood count, chemistry profile, and urinalysis performed as a routine part of the evaluation. |
Cushing’s disease can present with a variety of symptoms and may also be involved with several different disease processes. Therefore, it is recommended that any dog suspected of having Cushing’s disease should have acomplete blood count (CBC), blood chemistry panel, andurinalysis performed as a routine part of the evaluation. Common abnormalities in these tests include increases in alkaline phosphatase, and ALT (liver enzymes), increased cholesterol, decreased BUN (a kidney function test), and dilute urine (low specific gravity).
There are several different tests that can be performed to get a definitive diagnosis of Cushing’s disease. Many times the veterinarian may perform more than one test to help confirm the diagnosis or to determine which form of the disease is present. A diagnosis of Cushing’s disease, however, should never be made on the basis of laboratory tests alone. The dog needs to be showing symptoms of the disease, and have a medical history consistent with the diagnosis.
The three most common “screening” tests are the urine cortisol:creatinine ratio, the low dose dexamethasone suppression test, and ultrasound.
Urine Cortisol:Creatinine Ratio: In this test, the owner generally collects a urine sample at home (where the animal is not stressed). The sample is sent by the veterinarian to a special laboratory for testing. Most dogs with Cushing’s disease have an abnormal result. However, there are other diseases that can also cause abnormal results. So if this test is abnormal, further diagnostic testing should be performed.
Low Dose Dexamethasone Suppression Test: The low dose dexamethasone suppression test is useful in diagnosing Cushing’s disease in dogs. When given low doses of dexamethasone, normal dogs show a marked decrease in blood cortisol levels when tested 8 hours later. Most dogs (more than 90%) with Cushing’s disease do not have a decrease in cortisol level after being given dexamethasone. The results can sometimes help determine which type of disease is present.
ACTH Stimulation Test: This is another test that is commonly used in the diagnosis of Cushing’s disease today. It will not distinguish between the two types of hyperadrenocorticism, but it may aid in the diagnosis in difficult cases. It is also used to evaluate the effectiveness of therapy.
Abdominal Ultrasound: Abdominal ultrasound is helpful in three respects. First, it is a good test to evaluate all of the abdominal organs in the dog. Secondly, it is used to study the size and shape of the adrenal glands. The adrenal glands in pituitary dependent hyperadrenocorticism are usually normal in size or enlarged. If a tumor is present however, one adrenal gland is often abnormally large or of uneven shape. Finally, if a tumor is suspected, ultrasound can help identify any metastasis to other organs.
High Dose Dexamethasone Suppression Test: This blood test, which is not used often, may help to is used to distinguish between pituitary dependent hyperadrenocorticism and adrenal-based hyperadrenocorticism.
Treatment
Treatment consists of several different options. Depending on the type of disease, surgery can be performed. If an adrenal tumor is identified, then surgical removal may be a viable option. There are several different forms of tumors that can invade the adrenal gland and their treatment will be based on the particular tumor type.
Non surgical treatment is the most often used treatment for most cases of canine Cushing’s disease. About 80% of the cases of Cushing’s disease in the dog are of the pituitary type, and since both the adrenal and the pituitary type will respond effectively to some of the oral treatments, many veterinarians do not perform the diagnostics necessary to distinguish between the two different forms. There are currently several different oral medications being used to treat canine Cushing’s disease.
| Nonsurgical treatment is the most common treatment for canine Cushing’s disease. |
Lysodren: Until recently, Lysodren (also known as mitotane, and o,p’-DDD) was the only treatment available for pituitary dependent Cushing’s disease. It is convenient to use and is relatively inexpensive and is still probably the most widely used treatment. The downside of this drug is that it can have some serious side effects and regular blood-monitoring needs to be performed. During the initial phases of the therapy, the dog must be very carefully monitored, and there must be close communication between the veterinarian and the owner.
The use of Lysodren is somewhat like chemotherapy. It works by destroying cells of the adrenal gland that produce the corticosteroid hormones. As the number of corticosteroid-producing cells is reduced, even though the pituitary gland continues to produce excess ACTH, the adrenal gland is less able to respond, so the amount of glucocorticoid being produced is reduced. The problems arise when too much of the adrenal cortex is killed off. The animals may then need to be placed on prednisone, either short or long term. The Lysodren is initially given daily while the animal is being monitored for a decrease in the symptoms (water consumption, appetite). On the 8th or 9th day of the initial therapy, the dog needs to be examined and an ACTH stimulation test is performed to determine if the drug is working. If the goal is achieved, maintenance therapy is started. If the goal has not been reached, then the dog generally remains on the daily medication for 3 to 7 additional days and is rechecked until the proper results are achieved. If the dog becomes lethargic, vomits, or has diarrhea, or if the treatment does not work by 30 days, then the treatment plan is reevaluated. If treatment is successful, then symptoms should resolve within 4 to 6 months. A certain percentage of dogs will relapse and need to undergo the daily therapy again at some point in their lives. If a dog ever becomes ill while on Lysodren, the Lysodren should be stopped immediately and the dog should be examined by a veterinarian. If the therapy is successful, the dog will need to be on Lysodren for the rest of his life.
Trilostane: Trilostane is a newer treatment that is used to treat some dogs with Cushing’s disease. It is more expensive, but may be an alternative treatment for dogs with adrenal tumors. As with Lysodren, the dog is reexamined repeatedly during the initial phase of treatment, and ACTH stimulation tests are performed. In many cases, after several months of therapy the dose needs to be increased.
Ketoconazole: Ketoconazole is an oral antifungal agent that has been used extensively since the mid 80s. One of the side effects of ketoconazole is that it interferes with the synthesis of steroid hormones. It therefore gained some popularity as a treatment for Cushing’s disease. However, it is rarely used today.
L-deprenyl (Anipryl): L-deprenyl (Anipryl) has been advocated for the treatment of Cushing’s disease in dogs, but its effectiveness has come into question.
Summary
Cushing’s disease is a disease that affects middle age to older dogs. The affected animal has a characteristic presentation including increased water consumption and resulting increased urination, increased appetite, hair loss, and a potbellied appearance. There are several diagnostic tests available, as well as several treatments.
References and further reading
Bonagura, J. Kirk’s Current Veterinary Therapy XII. W.B. Saunders Co. Philadelphia, PA; 2000.
Feldman, EC. An update on the diagnosis of Cushing’s Syndrome in Dogs. Presented at the Wisconsin Veterinary Medical Association Convention, Madison, Wisconsin, October 2005.
Feldman, EC. Treatment of hyperadrenocorticism in dogs. Presented at the Wisconsin Veterinary Medical Association Convention, Madison, Wisconsin, October 2005.
Ramsey I, Neiger R. Canine hyperadrenocorticism. In: Bonagura JD, Twedt DC (eds.) Kirk’s Current Veterinary Therapy XIV. WB Saunders Co, Philadelphia, PA 2009:2224-227.
Reprinted as a courtesy and with permission from
PetEducation.com (http://www.PetEducation.com)
On-line store at http://www.DrsFosterSmith.com
Free pet supply catalog: 1-800-323-4208

How do you go about getting the scottish terrier health network app. Do you have an app to download…..ms. Becky
We’ve not got one yet, but you’ve given me the idea now! We’ll get back to you shortly.
Sent from my iPhone
Pingback: One Step Back | Scottie Mom·
Very informative article. I had recently taken an online course on canine hyperadrenocorticism (the other OTHER name for cushing’s disease) and this was a very useful supplement read.
I lost a lovely purebred wheaten Scottie to Cushing disease. That Scottie came to me from a reputable Scottie Rescue in Northern California. It was not diagnosed earlier or he might have lived longer. He died at almost 7 years old. His fur was very thick and did not look like he was shedding too much, he looked fat but his belly felt very hard to the touch, which is a bad sign, and I would like to add that another sign to be alerted to is if the dog seeks cool places where to lie; the vet told me it was the disease which makes them feel hot. My babe did not want to sleep on blankets but always preferred the tile floor. He was treated for two years by the best veterinary clinic in Northern California and then died in his sleep.
We are not even sure what occurred with our Miss Maggie. All we were told by The Vet, was her kidney values were way beyond bringing down to normal range.
She was on IV and I feel she had Cushing’s Disease that came about 5 years earlier. She had the hair loss and the “pot belly” look. She was house broken yet she would drink till no water was left. Of course hundreds of urinal accidents occurred. I suppose hindsight is 20/20 and we still feel guilty for her death.
Our 6 year old will receive a complete work up ASAP as my heart just can’t take another loss.
Thank you
My sweet lady has just been diagnosed – she is 10 years old abd tomorrow I start the ‘induction’ period. I am absolutely terrified of this. This Lysodrem sounds so lethal if you cannot even touch them without a glove? Any positive stories/cases please…I NEED TO BE POSITIVE.
Hi, yes the Lysodren medication does seem quite ‘serious’. Mostly here in the UK I’ve only read about scotties being given ‘Vetoryl’. Perhaps it’s different where you live? Perhaps have another word with the vets to ascertain the reasons why. You have the right to ask the questions, as you need to be sure what to look out for should there be a ‘reaction’ to the treatment. I’ll put this query onto the Facebook page to see what others think about the Lysodren route. Please keep in touch. Big hugs being sent to you and your sweet lady. Kx
Hi – thank you for the response. At the last minute I spoke to my vet to change to Trilostane (Vetoryl) – here in South Africa it is very very expensive, but I really don’t care about that – I would sell my soul for the girls. She is now on the 3rd day of it and so far…so good. I am watching her like a hawk, and she seems to be doing good. Many thanks – really appreciate the support.
Best Shirli
So pleased that you had the chance to discuss with your vet. The response from the Facebook posting was positive. If you didn’t get chance to read any of the comments, let me know and I’ll forward them onto you. Please do keep us posted as I’m now doing a little series of “Scotties living with Cushings” so you might feel able to contribute once the dosage has been sorted out. Have a great weekend and give your little girl and big hug from me. Kx
My Scottie is suspected to have Cushings. Been through the first round of evaluation and will do the second round next week. I am conflicted on whether to pursue the treatment or not.
The cost is of course a consideration but I also do not want to subject my boy to more agony
and uncomfortable treatments if not necessary. Has anyone tried the herbal choices? He as
of now has no hair loss. He looks fat, developed anxiousness, elevated thrist, accidents in the house, and panting. Makes be tear up to think of losing him and dragging out the inevitable if it is not going to work. Please Help. I
need input.
Hi Rebecca, thanks for dropping by. Sadly the cost of treatment for Cushings still remains high. However, Scotties are able to live a normal life once the right dosage has been determined. In fact scotties diagnosed with cushings at ages of 5 or 6 have live until 12+ and have passed away from unrelated conditions. I have looked into the herbal approach and will sort out the few documents I’ve been able to collect and send them to you in due course. Please bear in mind, that the herbal, or more natural course of treatments, all take much longer to establish themselves within your scottie, but the upside is that he will not have all those chemicals pumped into him. Bear with me whilst I get the relevant information across to you. I shall also ‘post’ this comment onto the Facebook Page – there should be quite a few useful comments you could consider and discuss with your vets. Regards, Karen x
Thanks for your reply. I am still anxious over what to do and am open to any info I can find.. Is the facebook page under scottie health of what? Please keep me posted of whatever you think will help me with my fellow. Thanks again.
Hi Rebecca – my little 10 year old girl is going for her 4th evaluation in two weeks. She has been on Trilostane for the second month now and the change has been remarkable. My vet and I are over the moon with the last results after just a month – she is far more comfortable, the thirst has stopped, the panting has stopped, she has lost a tiny bit of weight now and I can see she is feeling so much more comfortable. It is worth a try I reckon. All the best!
Thanks so much for you reply. The second evaluation came back with negative results from the lab as opposed to the first round of tests. We are waiting to see what develops. He had a good month but is suddenly more skiddish, eating more, drinking more and looks bloated. I can deal when he has the good spells but get so concerned when he appears to feel bad and displays some of the symptoms. Guess I just have to love him and be diligent.
Hi Rebecca – my little 10 year old girl is going for her 4th evaluation in two weeks. She has been on Trilostane for the second month now and the change has been remarkable. My vet and I are over the moon with the last results after just a month – she is far more comfortable, the thirst has stopped, the panting has stopped, she has lost a tiny bit of weight now and I can see she is feeling so much more comfortable. It is worth a try I reckon. All the best!
My Murphy is on herbal supplement called Ophiopogon Formula from my veterinary at FL Wild Veterinary Hospital 386 734 9899 He’s been taking this for a couple ofyrs now and is doing wonderful he will be 11 in March Praying you still have your Rebecca
Thanks for the encouraging info. He was a rescue. I have had him about 5 years and I had never heard of Cushings.. I was devastated reading about it after asking the vet to check him for diabetes etc due to his extreme thirstiness. Your info gives me encouragement to get through the next round. Thanks for taking the time to reply and help me
know there is hope.
Hello, our Scottie Dougie has been diagnosed diabetic and is having twice a day insulin injections. His thirst has not really settled at all so I questioned whether he had cushings. After an afternoon of the most awful stress to him at the vets having bloods, cannula inserted, getting so distressed and needing to be muzzled and still biting the vet, the first result came back as having diabetic stress, but the vet said going by his symptoms he has cushings but needed another test, done over 12 hrs. After much discussion with our family and the vet, we have decided not to go ahead with the second lot of tests as it is far too distressing for him and will need constant monitoring until his levels are acceptable….more procedures and blood tests . He is insured so it’s not a cost issue, it’s a case of keeping him comfortable and ensuring I can give him his insulin, because as it is now, following the first lot of test he has become more anxious with me when I give his injections and I can’t risk him becoming so distressed that I can’t even give him the insulin. Hard call but I think the best one for our Dougie